Here’s how to identify if your child has eczema, how you can reduce the chance of them developing it and how to treat eczema, if they’ve been diagnosed.
Eczema (atopic dermatitis) is a common skin condition that often affects young children.
The idea of a baby’s skin being soft and smooth may be a myth if the results from a survey conducted by the Eczema Association of Australasia (EAA) are anything to go by.
Of the 4000 people surveyed, 66 per cent of the eczema diagnoses were before the age of two—in fact, more than half (52 per cent) were between zero and six months old.
So if your child has eczema—or you think your child does—you are certainly not alone.
Symptoms of eczema
Does you child have eczema or is it something else? The first thing to do is to determine their family history, as your baby’s eczema would likely have been inherited.
The following signs could mean your child is suffering from eczema:
- Rash, commonly found in creases of the body (elbows, wrists, neck, behind the knees)
- Itchy skin
- Scaly and dry skin
- Tiny blisters with clear liquid can form if your child’s eczema is severe
- Weeping skin is an indication that the affected areas has developed a bacterial infection
Signs can show up as early as a few weeks after a baby is born.
Dr Simone Kooke shares more about eczema in the video below
Causes of eczema
Eczema happens when a person’s body is unable to effectively repair their skin barrier after it has been exposed to allergens or irritants. The skin therefore loses moisture, causing it to become dry, scaly, red and itchy.
Eczema is a skin condition that’s related to other allergic conditions including asthma and hay fever. Children with eczema may also develop these conditions or food allergies later in life.
Some, however, may never know the real reason behind their condition.
Alicia Preston’s daughter, Poppy, was just 11 weeks old when she was diagnosed with eczema by her paediatrician.
“The first 11 weeks of her life, Poppy’s skin was beautiful and perfect,” recalls Alicia, who lives on Queensland’s Sunshine Coast.
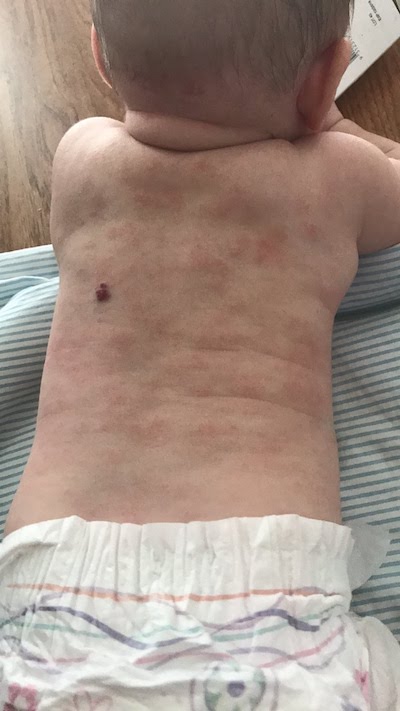
While the real cause of Poppy’s eczema is unknown, doctors suspect a gastrointestinal virus may have changed the stomach lining of 11-week-old Poppy, resulting in a flare-up.
“But it’s also possible she was always going to get eczema and it just coincided with her falling sick,” says Alicia, who prior to Poppy’s diagnosis, never had much exposure to eczema.
For the next five to six months, Alicia struggled to keep Poppy’s eczema under control—it affected her baby from head to toe.
“She didn’t sleep because she was scratching. I had to lie in bed with her and hold her arms away from her body,” says Alicia. “Everything I did to try to control it just didn’t work.”
Ten-year-old Ryder Taylor had a similar experience when at four months old, he woke up with what his mum Michelle thought then was a rash all over his body.
The family had never experienced the effects of eczema in their lives prior to youngest child Ryder, so the diagnosis came as a bit of a surprise.
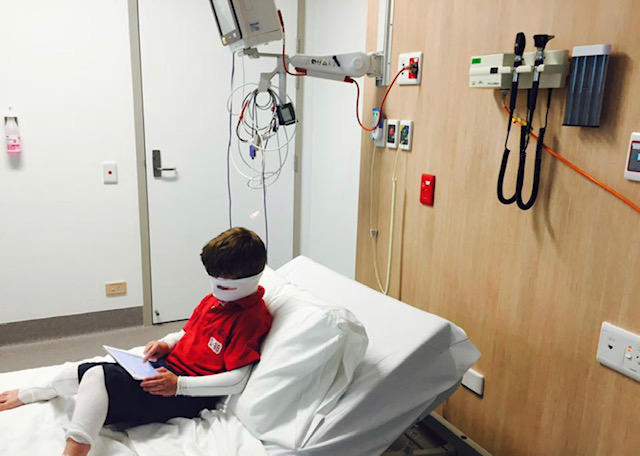
“We waited months for specialist appointments to educate ourselves on how to care for our baby, who was red-raw and covered in eczema breakouts, especially on his head,” says Michelle.
“My nights consisted of putting socks on Ryder’s hands [to use as mittens] to stop him scratching and waking up regularly to apply lotions on him. I remember his sheets being covered in blood from how badly he scratched himself.”
How to reduce your baby’s chances of developing eczema

While it may not be entirely possible to completely stop your baby from developing eczema, there are certain things you can do to help reduce their risks after they’re born.
- Don’t bath babies every day as it will strip off any natural oils protecting their skin
- Use fragrance-free cleansers
- Avoid soap-based products and bubble baths. Bath oils or even coconut or olive oil are better
- No hot baths. Use lukewarm water or warm water instead
- Regularly use moisturisers
Pregnant? Dr Simone has some tips on what you can do now to help your unborn baby’s skin
Common triggers of eczema
Identifying what triggers your child’s eczema is crucial when it comes to being in control of their skin condition, and preventing an eczema flare-up. These include:
- Exposure to dust and dust mites
- Pollen and grass
- Animals
- Sensitivity to certain types of food, such as dairy
- Change in weather, especially in the lead-up to winter
“The cleanliness guidelines to prevent the spreading of COVID-19 is a concern for those with eczema,” says EAA president Cheryl Talent. “The emphasis on cleanliness has proven a trigger for a lot of sufferers due to their sensitive skin and not understanding which hygienic products to use.”
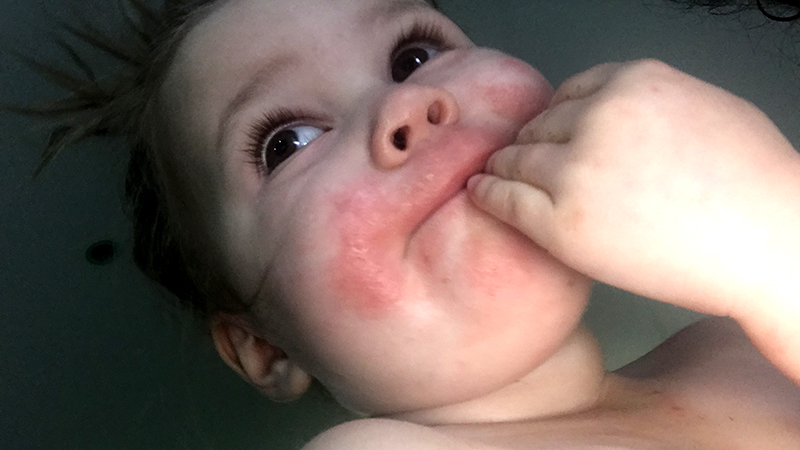
For Alicia and young Poppy, the turning point came when Poppy was nine months old.
“There is a lot of misinformation surrounding eczema. The best thing I did was to start seeing dermatologists and specialists who dealt with infant eczema. I now know what to do straight away,” says Alicia. “Eczema doesn’t scare me anymore.”
Eczema treatment options
Over-the-counter treatment options and even just increased skin care and moisturising can often help with a mild eczema rash. It’s important to chat with your GP to determine the best treatment plan for your child, especially in more serious cases.
In Alicia and Poppy’s case, treatment included:
- Bleach baths
- Wet wraps
- Steroid injections
- Cortisone or steroid cream
- Topical antibiotics
Poppy is now four and Alicia is also very careful with the type of laundry detergent and cleaning products she uses. She is vigilant about regularly changing Poppy’s bedsheets and vacuuming, as well as having the house professionally cleaned every six months.
“It’s hard and there will be sleepless nights watching your child rip at themselves,” says Alicia, “but be strong and you will make it work and it will become a part of your normal life. Once you get a good team of specialists around you and a good routine for your child, and find out what works well for your child’s skin, it takes a big load off. It may take 12 months or four years, but you can treat it and you will get there.”
Dispelling common eczema myths
according to the EAA

Myth: Eczema is contagious
Eczema is not contagious, which means you can’t “catch” the disease from another person and you can’t give it to someone by touching them.
Myth: Eczema is like acne
Eczema and acne are completely different conditions. However, it is true that some medications may cause acne and complicate eczema.
Myth: People who have eczema do not wash properly
Having eczema has nothing to do with personal hygiene; the disease is believed to be caused by a combination of environmental, genetic and immune system factors.
Myth: Eczema will leave permanent scars
Generally, no. Although eczema can be very uncomfortable and unpleasant, it is unusual for it to leave any permanent marks on a person’s skin.
Myth: Eczema can be cured with steroids
Unfortunately, there is no cure for eczema. Although steroids have been used for a long time to treat eczema, they are not a cure and there are limitations for treatment.
This post includes affiliates and/or paid inclusions.
Any advice given is general in nature and is not intended as a substitute for medical advice and must not be relied upon as such. For any healthcare advice, always consult a healthcare practitioner.
How helpful was this article?
Click on a star to rate it!
0 / 5. 0
Be the first to rate this post!
Melody Tan
Related posts
Subscribe
Receive personalised articles from experts and wellness inspiration weekly!


